Our AI claim agent scrubs CPT, ICD-10, and HCPCS codes against live payer edits at the point of submission. It also identifies prior authorization gaps, modifier errors, and auto-generate appeals through real time AI claim processing.
Book a Free Demo
Trusted by 1000+ providers

Reduction in Denial Rate
Autonomous Claim Monitoring
Faster than Manual Submission

Health insurance companies have developed AI that reviews clinical documentation, finds coding gaps and triggers denials instantly. In the last couple of years, denial rates went up to 15% with 25% of the providers reporting the increased denial rate was entirely due to payer-side automation. The reality is that manual workflows are basically outmatched at every stage of the claim lifecycle. That’s where AI claim processing comes in. Our AI claim agent is your best bet. It automates the entire claim lifecycle and results in faster claim submission, 98% first-pass acceptance, and 40% less denials.
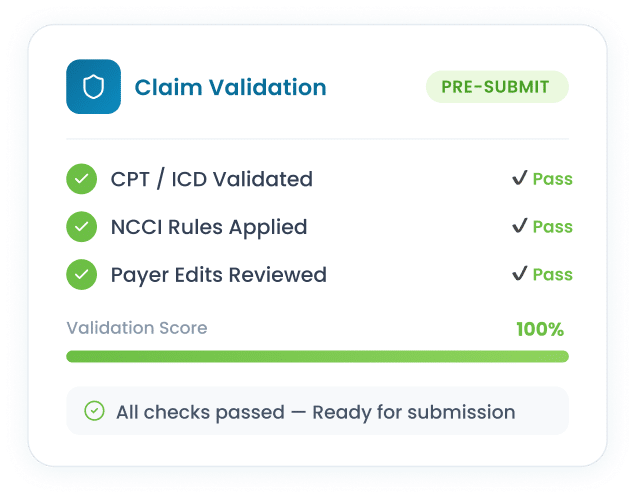
Our claims processing automation starts with an audit of every claim against live payer-specific edits, CPT/ICD-10 code validation, and NCCI rules. All this happens before the claim is submitted.
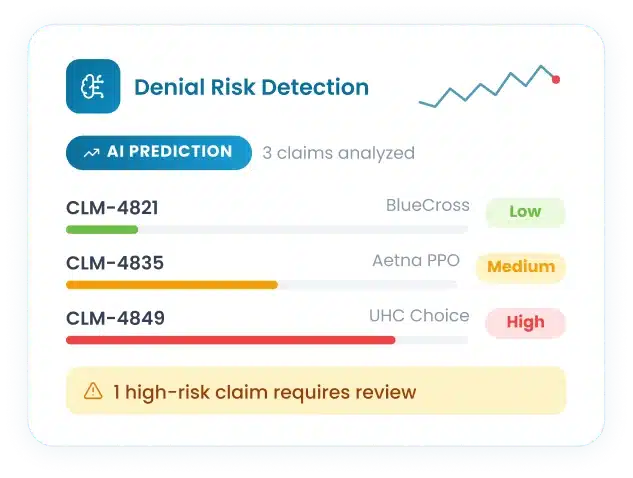
Through machine learning, the claim agent flags high-risk claims and prevents them from getting submitted. It also analyzes payer behavior and denial patterns to reduce denials.
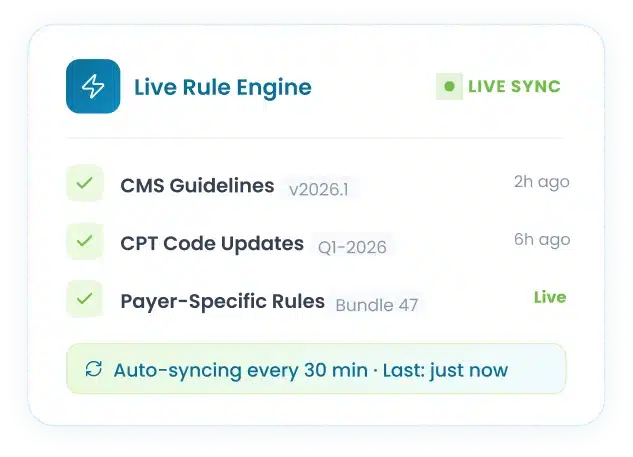
The AI agent continuously updates itself against CMS guidelines, AMA CPT changes, and all payer-specific edits in real time through automation. This way every claim is checked against the latest rules and policies.
NLP is used to review clinical notes against the payer’s medical necessity criteria and flags documentation gaps before submission. As a result, you get a correction notification instantly, not a denial later.
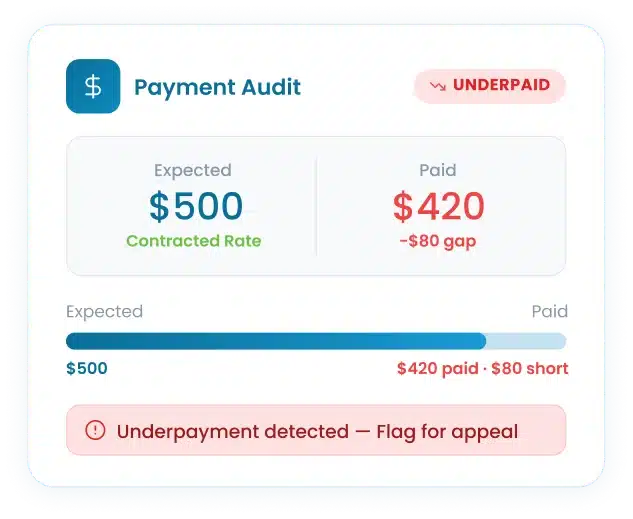
Every posted payment is automatically cross-checked with your contracted rates to find any underpayments before they are submitted. All discrepancies are flagged and escalated in their window.

Our AI claim agent helps you submit a claim fully automated with an end-to-end process that validates, tracks, and recovers revenue. Here’s what our claim agent can do for you through AI
The claim agent verifies patient coverage, copays, deductibles, and authorization requirements autonomously in real time. If there are any errors, the agent flags and resolves them instantly.
Our AI claim processing agent detects the authorization requirements as per the procedure and payer, collects documentation from your EHR, and submits the authorization request automatically.
Once a claim is validated, it’s compiled, formatted to ANSI X12 837 standards, and electronically transmitted to the appropriate payer. This way the claim gets approved the first time.
The AI agent monitors every submitted claim across all payers simultaneously and flags any exceptions the moment they occur. All this without any portal login or error.
There’s a slim chance but if a denial happens, the AI will read the CARC and RARC codes, identify the root cause, and build a payer-specific appeal using clinical documentation.
ERA remittance data is matched to submitted claims and payments are posted without any reconciliation. Also, the AI agent cross-references all the payments against the contracted rates.
Join 1000+ providers who have reduced denials and cut authorization time by 70% with MedCare MSO
Every specialty has its own payer rules, documentation standards, and modifier requirements, which our AI claim agent is trained on.

Our claim agent can connect directly to your existing EHR via HL7, FHIR, and secure API seamlessly. It can access clinical documentation, patient demographics, and payer information in real time without any disruption.
















The AI Claim Agent has completely changed how we handle denials. It catches errors before submission, flags underpayments automatically, and even generates appeals without manual effort. Our reimbursement speed has improved significantly.
What stands out is the accuracy. The system checks claims against payer rules instantly and prevents avoidable rejections. It has made our billing workflow much more predictable and efficient.
We used to spend hours on prior authorizations and claim follow-ups. Now the AI Claim Agent manages everything in real time. It’s reduced our denial rate and helped us recover revenue we were previously writing off.
An AI claim agent is an autonomous system that takes care of the entire claim lifecycle. It includes claim scrubbing, submission, tracking, appealing, and posting without any manual intervention. There’s NLP and ML behind its validation and it uses CARC and RARC code logic for problem resolution.
Yes, the AI reads CARC and RARC codes, cross-checks the policy rules, and identifies root cause patterns across the claim batch. This way it identifies and handles multi-payer denials in a single go.
The AI claim processing includes the capability to automatically detect whether prior authorization is required or not. It checks procedure & payer, collects clinical documentation from the EHR, submits the request, and tracks the status.
It happens rarely but when it occurs, we have in-house professionals who take care of the escalated claim. What happens is the AI escalates the claim by flagging it, preparing a complete case summary, and routing it to the appropriate specialist.
The AI scrubs every claim against payer edits, NCCI rules, and validates codes before submitting. This way it catches errors that would otherwise result in a denial. Also, machine learning identifies historical data and makes decisions from it which results in reduced denials.
Ready to maximize your revenue while reducing administrative work? Let’s team up! Our medical billing expert will reach out within 12 hours.
Please provide the following information, so our team can connect with you within 12 hours.
Or call us as 800-640-6409