Our AI medical billing software scrubs claims in real time using built-in and practice-specific engine rules to ensure pre-submission compliance. It automatically detects and resolves errors, reducing denials and maintaining steady revenue flow.
Request a Demo
Trusted by 1000+ providers

Automatically identifies and corrects common coding issues like CPT/ICD mismatches, modifier conflicts, NCCI edits, and more before submission. It eliminates claim errors and improves the first-pass acceptance ratio.
Prevent recurring denials by implementing dynamic, payer specific rules for Medicare, LCD/NCD compliance, commercial payers, and more. It stops the cycle of denials with intelligent, automated logic.
Our AI Rule Engine analyzes denial patterns, automatically adjusting rule logic to prevent the same issues from recurring. By identifying root causes of denials, it continuously updates its processes, applies auto actions, and eliminates the need for manual corrections.
Our AI Rule Engine guarantees strict adherence to CMS guidelines, practice SOPs, and specific rules. By automating compliance checks, it reduces audit risk and enhances operational accuracy across your billing processes.
Empower your billing team by automating error detection and claim validation. Our AI Rule Engine takes over the tedious tasks, ensuring claims are accurate and ready for submission without constant human oversight.
Ensures full adherence to payer specific guidelines, including LCD/NCD rules, NCCI Edits, MUE, Medicare policies, and contract requirements. It automates compliance to reduce rejections and increase first pass claims submission rate.
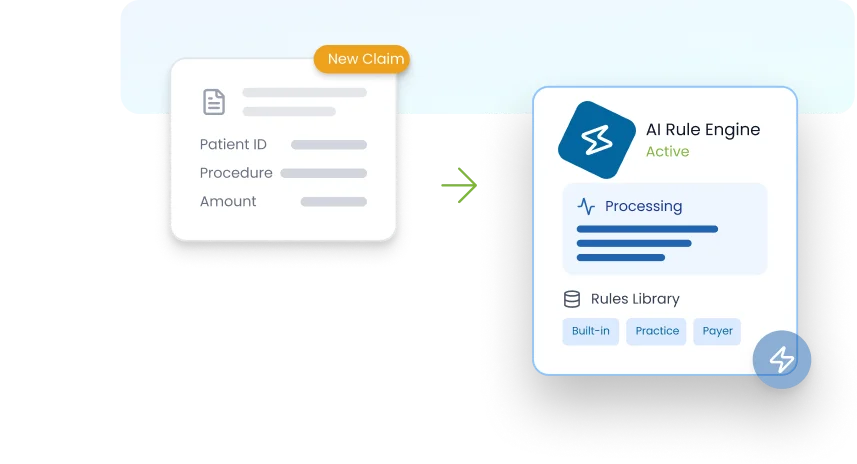
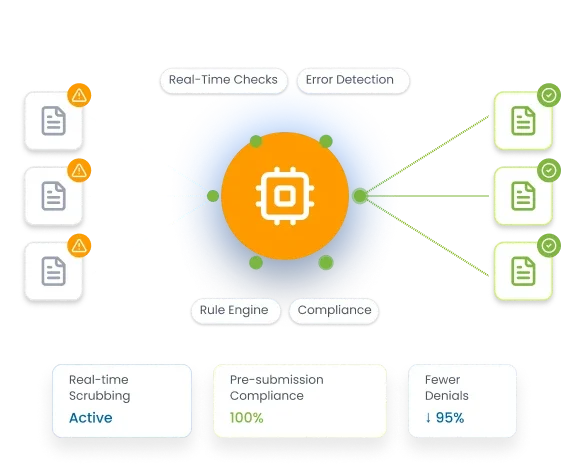
Before the submission of the claim, the AI rule engine automatically triggers the required rules.
Global and practice-specific rules run automatically, checking compliance, eligibility, coding logic, and payer requirements.
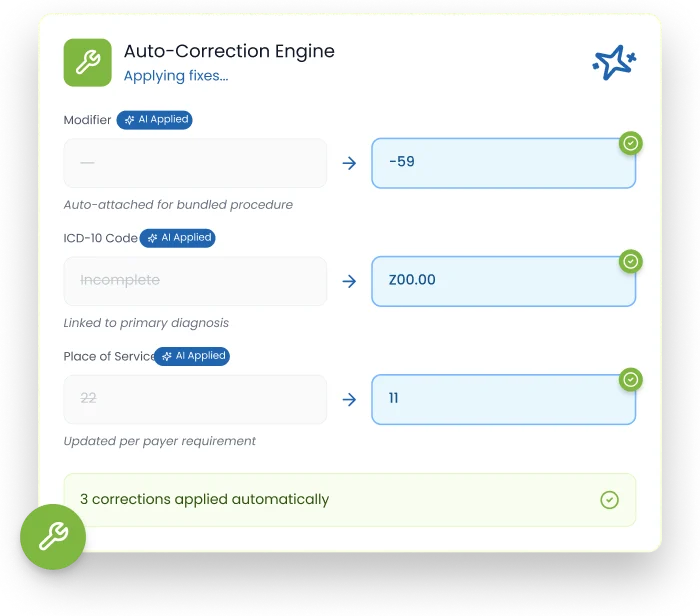
The system applies auto actions such as modifier attachment and ICD linking to fix eligible errors in real time.
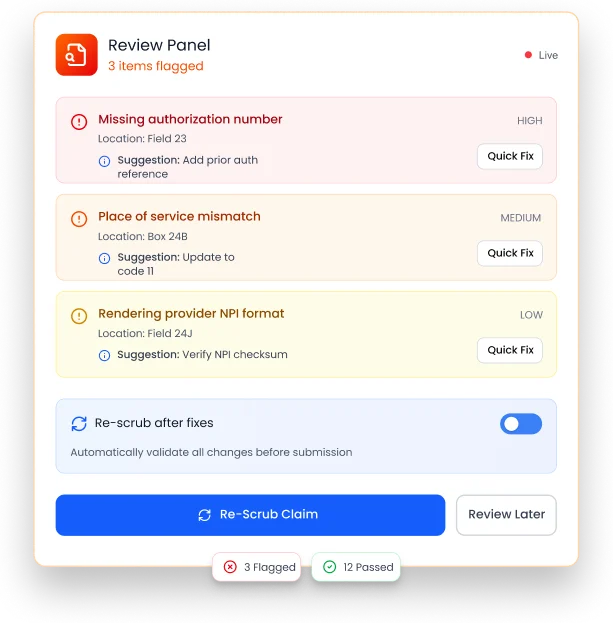
Any remaining issues are clearly flagged for review, corrected by the billing team, and rescrubbed instantly.
Only fully validated, compliant claims are released to the clearinghouse, while unresolved claims move to a tracked rejection queue.
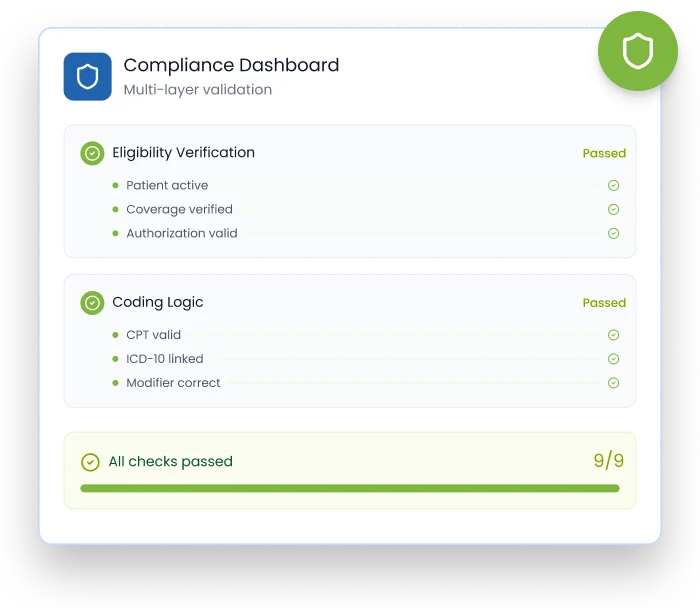
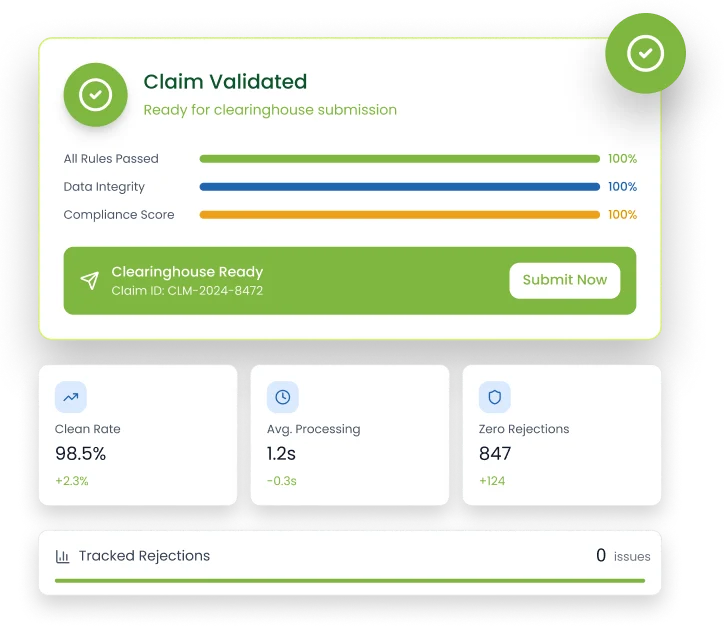
Billing teams often submit claims without visibility into payer specific conditions, enrollment status, or coverage constraints, only discovering issues after the claim is rejected. The AI rule engine evaluates these variables at submission, enforcing payer logic in real time so only compliant, submission-ready claims move forward, which increases the first pass clean claim rate by 98.5%.
Revenue is often lost when subtle coding conflicts or non-standard payer requirements go unnoticed until after payment is delayed or reduced. The rule engine AI scrubber software applies paye specific and custom logic upfront, identifying these risks early and ensuring claims align with reimbursement rules before submission.
The AI Rule Engine automatically corrects common claim errors, reducing the need for manual intervention. For example, if a modifier 25 is required, the engine automatically places it in the claim. Similarly, if a POS code is missing or incorrect, the engine auto corrects it based on the claim's details, ensuring compliance and reducing claim errors without manual effort. This leads to faster claim submissions.
Billing rules often change, vary by payer, and differ across practices, making manual enforcement unreliable and inconsistent over time. Our AI rule engine is built on a governed rule lifecycle. Rules are defined with clear intent, mapped to payer policies, tested against real claim scenarios, approved through controlled workflows, and then deployed into production. Once active, these rules continuously monitor claims, apply logic driven validations or corrections, and are reviewed, versioned, or rolled back as policies evolve, ensuring long-term accuracy without disrupting billing operations.
Our AI rule engine is built for 50+ medical specialties:
Our AI Rule Engine ensures compliance with CMS, LCD/NCD policies, NCCI edits, Medicare Part B rules, DME MAC logic, vaccine guidelines, and payer-specific billing rules, with continuous updates for regulatory changes
Maps rules to specific payers, applies coverage rules by Date of Service, and validates medical necessity. Tracks policy revisions and ensures your practice remains compliant with evolving healthcare regulations.
Generates detailed decision logs, traceability, and policy references for each rule execution. This ensures defensible documentation during internal audits, payer reviews, and external regulatory inspections to support continuous compliance.
Our solution features role based access control, rule version management, change approval workflows, and environment separation (Dev/Test/Prod), ensuring governance and compliance for enterprise-level organizations across all operations.
The AI Rule Engine supports HIPAA aligned billing operations by enforcing secure transaction validation (837P/837I), maintaining role based access, and generating audit ready logs, helping protect PHI while reducing billing errors and compliance risk.
Since implementing the MedCare AI billing software and its AI rule driven engine, we’ve caught documentation-to-code mismatches before submission, which significantly reduced denials and time spent on rework. The coding validation and claim quality checks have improved our clean claim performance and made our billing process far more predictable.
The rule engine catches payer specific issues we used to miss. Our first pass acceptance improved, and compliance checks now happen automatically without extra effort.
The auto actions and exception only workflow save our billing team hours every week. We spend less time fixing routine errors and more time on real issues.
Unlike basic medical billing software, our AI rule engine supports governed rule logic, practice specific rules, auto actions, and real time validation before claims reach the clearinghouse.
No. The scrubber runs within the existing workflow, validates claims in real time, and reduces manual review, improving speed without adding steps.
Yes. Rules can be updated, versioned, tested, and redeployed as payer policies evolve, without disrupting live billing operations.
Rule creation and deployment follow role based controls, ensuring only authorized users can design, approve, or activate rule logic.
Rules can be paused or rolled back immediately using built in rollback controls, protecting active claims and revenue flow.
Pricing is based on usage, practice size, and rule complexity. We offer flexible plans that scale with claim volume and customization needs.
Ready to maximize your revenue while reducing administrative work? Let’s team up! Our medical billing expert will reach out within 12 hours.
Please provide the following information, so our team can connect with you within 12 hours.
Or call us as 800-640-6409