Every claim in Texas starts a 95-day countdown. Miss that filing deadline or slip up on a single data point like an NPI, taxonomy code, or diagnosis pointer, and the claim bounces back while the clock keeps running. Add January’s fresh CPT and ICD-10 code sets, weekly prior-auth changes, and a jumble of Medicare, Medicaid, TRICARE, and HMO edits, and even the best in-house team can stall out. Cash piles up in limbo, staff scramble, and revenue slows.
That’s when many practices call in outside help. The right billing partner tracks every code update, auto-checks eligibility, locks down prior authorizations, and appeals denials before they dent cash flow. This blog post introduces the top 5 medical billing companies in Texas that do exactly that, beat the 95-day rule, slash rejection rates, and turn red “DENIED” stamps into steady green deposits.
Quick-Glance Comparison Table of the Best Medical Billing Services in Texas

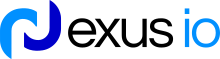
Here’s a list of the top 5 medical billing companies in Texas. We’ll explain what each one does, highlight its expertise, and show why it’s a smart choice for the healthcare practices, labs, and clinics in Texas that need faster, more accurate payments.
MedCare MSO ranks among the top medical billing companies in Texas, serving practices across every major metro from Dallas-Fort Worth to the Rio Grande Valley, while supporting more than 50 clinical specialties. Working on a pay-for-paid model, it hits the state’s 95-day filing clock, automates eligibility checks, stays current with every CPT and ICD-10 update, masters prior authorizations, and crushes denial backlogs to drive real revenue growth. The firm also installs billing software and handles denied-claim appeals at no extra cost, and its credentials include HIPAA compliance, ISO 9001:2015 certification, a BBB A+ rating, AAPC Education Provider status, and memberships with ASRM and NILA.
Experience: 13+ Years
Location: Texas
MedCare MSO powers a fully electronic billing cycle, pulling charges directly from the EHR through proactive integrations and routing them through an intelligent scrubber for CPT/ICD-10 and NCCI edits before end-to-end EDI/ERA submission, so payments land in 7–14 days. It’s pay-for-paid, risk-free model that aligns incentives providers owe nothing until collections post, while real-time eligibility checks, prior-authorization automation, and claim scrubbing slash “no-coverage” denials and trim aged A/R. Layer in all-inclusive Texas compliance and support covering HIPAA, No Surprises Act, and state prompt-pay laws, plus Texas-specific MIPS dashboards and credentialing alerts, and labs enjoy cleaner claims, faster cash flow, and worry-free oversight.
Work with billing experts who understand your specialty-specific rules, payer requirements, and documentation standards to accelerate reimbursements and reduce revenue leakage.
PUREDI is a 100 % cloud-based revenue-cycle partner that has spent more than two decades helping Texas physicians, practices, and management groups turn clean claims into faster payments. Its intelligent software pairs with a team of seasoned billers and coders who audit every claim line, work with multiple clearinghouses to keep submissions flowing even during outages, and deliver free analytics that pinpoint denial root causes. Grounded in strict compliance and ethical standards, PUREDI’s end-to-end service lets clinicians focus on patient care while it drives measurable gains in reimbursement and cash flow.
Experience: 20 Years
Location: Austin, TX
PUREDI stands out among RCM providers Texas trusts because it pairs a real-time error checking and denial prevention engine, boosting a 93% first-pass acceptance rate, with built-in physician-billing consulting that drives denials down month after month. Their cloud platform flags coding errors before claims leave your office, then routes any stubborn issues to human experts for same-day fixes and clear coaching. Additionally, robust dashboards, mass-action tools, and an integrated clearinghouse let hospitalist groups, multispecialty practices, post-acute providers, and even other billing companies scale effortlessly. In short, PUREDI turns raw billing data into targeted guidance and faster reimbursements without adding extra staff.
Dastify Solutions is an independent, ISO/IEC 27001:2013-certified revenue-cycle ally that provides “the future of medical billing” to all healthcare sizes. With the combination of staff augmentation, operations consulting, and end-to-end billing integrated with analytics-driven workflows, their global staff automates back-end functions, decreases denials, and increases clean-claim rates, allowing practices, FQHCs, hospitals, and surgical centers to focus on patient care and financial independence. Meanwhile, each interaction is tailored, data-protected, and rooted in relentless improvement, so you witness cash leaks plugged and revenue moving more quickly.
Experience: 5 Years
Location: McKinney, TX
Dastify Solutions ranks among the top revenue cycle management Texas providers. The company unites end-to-end RCM muscle under one roof, with physician-billing teams that file claims quickly and accurately using advanced automation. Its oncology coders master complex CPT/HCPCS rules, DMEPOS and HME specialists apply payer nuances to capture every allowable dollar, and a dedicated eligibility-and-authorization desk verifies benefits up front to prevent coverage snags.
All that data feeds a metrics-driven A/R and denial-management engine that consistently wins first-pass adjudication, shrinking overhead, lifting collections, and cutting write-offs for solo providers, large groups, and new practices alike.
Nexus io is a leading AI-powered revenue cycle management (RCM) and medical billing company headquartered in Phoenix, Arizona. Nexus io uses AAPC certified coders in combination with proprietary artificial intelligence technology to automate various components of Revenue Cycle Management (RCM) for providers. These components include real-time eligibility verification, automated claim scrubbing, predictive denial flagging, concurrency detection, accounts receivable recovery, credentialing, and reporting.
Nexus io services all sizes and types of medical practices in all 50 states. The company offers seamless integration into existing EHR and PMS with 24/7 support as well as an average onboarding time of 30-45 business days.
Experience: Over 10 years (established 2015)
Location: Phoenix, AZ
Nexus io has an exceptional first-pass clean claim success rate of 98% (which is significantly higher than MGMA and other industry standards), a collection rate of 97%, and an average increase in revenue for new clients of between 20-30% during their first year. In addition, AI-driven automation within Nexus io detects and prevents errors before claims are submitted including missing time units, invalid modifiers, concurrency violations and place-of-service errors. Nexus io strives to reduce billing complexity, maximize reimbursement, assure regulatory compliance and allow providers to focus on delivering high-quality patient care through precision-driven RCM. The company maintains a strong reputation for reliability and client satisfaction.
Storm Medical Billing is an Austin business that has emerged as a top medical billing business in Texas, offering behavioral-health billing to therapists, psychologists, and other independent practitioners across the United States. Owner Carole Storm employs a HIPAA-compliant team that files and services claims through encrypted, SSL-secured transactions, coupling personalized service with sophisticated data protections to allow clinicians more time and receive the highest reimbursements.
Experience: 9 Years
Location: Austin, TX
Storm Medical Billing combines boutique-level attention with clear, cost-saving terms. Founder Carole Storm personally onboards every new behavioral-health client, clears any claim backlog, and tailors flat-rate pricing just $4.99 per date of service after a no-setup, two-month trial, so practices can forecast revenue without surrendering a percentage. A free 30-minute credentialing consultation streamlines newcomers into payer panels, and HIPAA-influenced security measures, including encrypted SSL links, layered firewalls, and audited access controls, guard each byte of patient data. The result is an open, secure association that enables therapists and psychologists to delegate billing worries and focus on patient care.
Choosing among the many medical billing companies in Texas comes down to fit: the partner must hit the state’s 95-day clock, master shifting CPT/ICD-10 edits, and keep you compliant with HIPAA, No Surprises, and Texas prompt-pay rules, all while giving you clear visibility into cash flow. The five firms profiled here show there’s no one-size-fits-all solution; instead, match the partner’s strengths to your own pain points, whether that’s pathology-heavy work, behavioral-health nuance, or rapid claim-turnaround at scale. Evaluate the data, talk to current clients, and make sure the service team, not just the sales deck, meets your expectations before you sign.
Work smarter, not harder—our platform improves every step of your process.
Please provide the following information, so our team can connect with you within 12 hours.
Or call us as 800-640-6409