The future of patient care is predictive analytics in healthcare, which allows healthcare providers to foresee potential health risks and patient needs and meet them before these issues develop. Due to the use of artificial intelligence and machine learning on large amounts of electronic health data, hospitals can predict complications or readmission risks before they occur. This shift from reactive to proactive medicine has shown real impact in one example, a hospital system cut its $4.2 million annual preventable readmission costs in half within 18 months of implementing predictive analytics. Practically, predictive analytics can help clinicians to customize treatment, schedule preventive follow-ups, and allocate resources more effectively to achieve better results and save costs on patients and healthcare organizations alike.
What is Predictive Analytics in Healthcare?
The use of statistical models and machine learning algorithms to analyze past and current patient data to make predictions about the future health events is known as predictive analytics in healthcare. In contrast to conventional reporting, which informs us of what has happened yesterday, predictive analytics provides estimates on the probability of such events as disease onset before they happen, readmissions, or treatment reactions. Practically, hospitals can gather data using EHRs, lab systems, insurance claims, patient monitors and even wearable devices and run the data through machine learning models. These models detect the hidden patterns such as combinations of lab values or vital sign trends of patients who can be predicted to be at high risk of complications or hospitalization.
The Predictive Analytics Framework
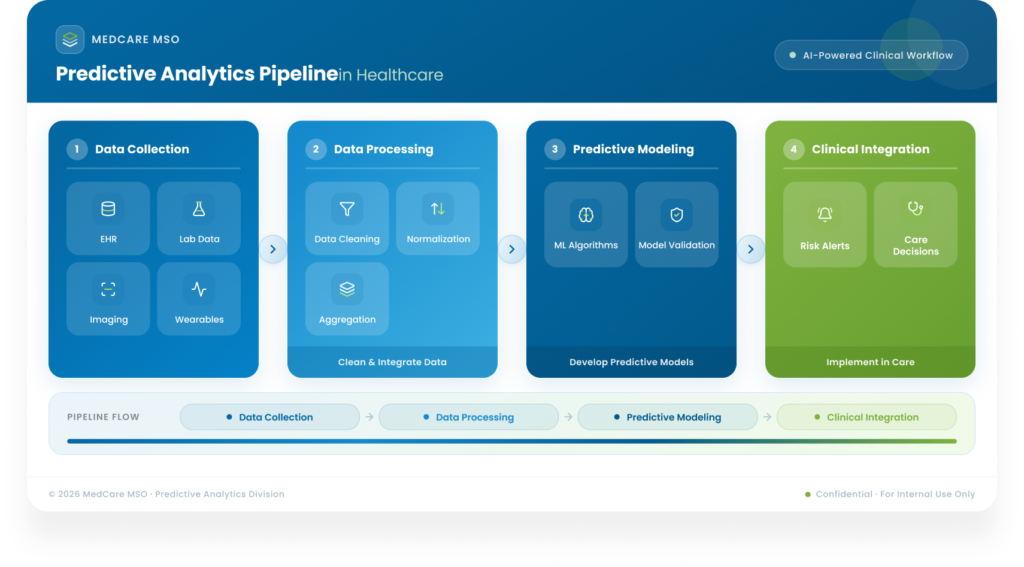
Implementing predictive analytics typically follows a multi-stage framework, each step critical to success:
Data Integration
Combine patient data across various sources (EHRs, labs, imaging, claims and wearables) into a single dataset. This is usually the most difficult part of the process, since the healthcare data is provided by 5-15 systems that can hardly speak with one language. It is common in hospitals to take months before cleaning up and matching records (e.g. fixing duplicates of patients) before the process of modeling can even start.
Data Preprocessing
These include the management of missing values, standardization of forms and organization of free-text notes. Models can only be trained after data is reliable.
Predictive Modeling
Feed the data that has been prepared through machine learning algorithms (e.g. logistic regression, decision trees, or neural networks). The model acquires the relationship (e.g. risk factors of readmission) based on past cases. The model is then checked against new patient data to test excellence and prevent any bias. Practically, simpler explainable models (so that clinicians place their trust in the results) are frequently the initial steps of the team and more complicated AI is introduced when confidence is established.
Clinical Action & Integration.
Implement the model in practice, such as the system could automatically calculate a risk score of every hospitalized patient. Clinicians can then rely on this insight to make decisions, including making a high-risk patient have more home visits. Retraining and continuous monitoring make the model accurate with time.
Benefits of Predictive Analytics in Healthcare
The benefits of predictive analytics in healthcare are wide-ranging and profound. By turning data into foresight, hospitals and providers can improve patient outcomes, cut costs, and streamline operations. Key advantages include:
Improved Patient Care & Outcomes.
High-risk patients are identified and the predictive models are used to intervene early. As an example, based on lab findings and vitals, analytics can identify the insidious signs of sepsis or worsening heart performance before the conventional observations. This early warning enables the care team to modify treatment or increase levels of monitoring, which can often stop emergencies.
Reduced Costs & Waste:
As healthcare budgets become stressed, analytics can be used to distribute resources where they are required. Models are able to predict demand and use of resources including determining the number of beds that will be required in future weeks depending on the epidemiological trends and other factors in the area. This does not cause overstaffing or holding of unnecessary stocks.
Enhanced Disease Control:
Behavioral disorders demand constant attention. Analytics will allow constant monitoring, wearable and home surveillance devices will send data to cloud models. The models are able to anticipate flare-ups in the conditions such as diabetes, COPD or asthma hence the care teams are able to intervene earlier.
Personalized Medicine:
Predictive analytics is the future of truly individualized care by taking clinical data and integrating them with genetic, lifestyle and environmental data. The models are able to propose an optimal treatment depending on the profile of a patient, reducing the trial and error of the standard care. In cancer diagnostics, such as oncology, predictive analytics uses tumor genetics to prescribe treatments that have the highest chances of success.
Proactive Population and Public Health:
On top of the individual, analytics helps in the public health. Through the de-identified population data (EHRs in combination with socioeconomic factors), health professionals are able to notice emerging diseases outbreaks or the communities in danger. They have been used to predict flu spikes or even monitor the spread of infectious diseases, meaning that they are able to predict beforehand and use this to launch a vaccination programme, or mobilize resources.
How Predictive Analytics is Applicable in Hospital Operations?
Besides direct clinical care, predictive analytics is changing the way hospitals function and perform financially. The hospitals can predict census through the analysis of historical admissions, seasonal patterns, and patient acuity and can proactively adjust staffing. This would aid in avoiding an issue of understaffing that would affect the quality of care and also over-staffing which would escalate the costs.
Predictive models are used in an emergency department to anticipate surges in patients and wait times to allow an administrator to bring in more staff or open fast-track lanes before the patient volumes become too large. The operation room schedules are streamlined based on the duration of activities and the surgeon schedules and minimized idle time and expensive overtime.
Predictive analytics enhances revenue cycle management by detecting the claims, which are likely to be denied, and the presence of coding gaps, prior to submissions, introducing a better reimbursement rate and cash flow. When integrated with AI medical billing software and advanced hospital billing services, these predictive capabilities further strengthen financial performance by automating claim validation, improving coding accuracy, and proactively reducing denials.
Moreover, predictive models contribute to increased engagement rates among patients because they determine those at risk of missing an appointment or needing outreach and provide the provider with the unique opportunity to intervene in the early stages and enhance continuity rates and the efficiency of the system, in general.
Addressing Healthcare Data Management Challenges Through Predictive Analytics with MedCare MSO
Challenges
Following are the healthcare data management challenges:
Information Quality and Consolidation
Healthcare information is usually divided into various systems like EHRs, laboratory systems, radiology systems, and billing software. These systems can employ the use of various formats, coding standards and names. Redundant, erratic or missing records lead to lower data reliability and may have a major influence on predictive model accuracy. Analytics initiatives are not able to deliver credible insights without robust data governance and integration systems.
Inadequate Technical Expertise
The creation of predictive analytics solutions presupposes the experience in the fields of data science, machine learning, healthcare informatics, and model validation. Lots of hospitals and groups of doctors do not have in-house analytics group that can create, test and support complicated models. Also, not only should models undergo constant monitoring and retraining, but also with changes in patient population and clinical guidelines.
Ethical Concerns, Security and Privacy
The information in healthcare is very sensitive and is highly controlled by laws like the HIPAA and GDPR. Organizations should make sure that there is secure data processing, encryption and restricted access. In addition to compliance, another issue is algorithmic bias because the models that are trained on an incomplete or unbalanced dataset may inherently perpetuate healthcare disparities. There should be ethical control and open validation procedures.
High Implementation Costs
Predictive analytics infrastructure can be an expensive undertaking in terms of software platforms, hardware, data storage, integration solutions, and human resources. The cost may be as low as hundreds of thousands or more than a million dollars depending on the initial costs. Smaller hospitals might not be able to afford such initial outlays, even where the payback of the investment is good.
Workflow Integration and Change Management
Predictive insights have to be incorporated into the daily clinical and administrative workflows to establish value. To incorporate analytics into work processes, sometimes staff training, system redesign, and culture adjustment is necessary. Even a highly accurate model can end up not used at all or not used fully without adequate change management and guidelines.
MedCare MSO can solve these issues by offering end-to-end healthcare data integration services, cutting-edge analytics skills, and secure and HIPAA-compliant infrastructure. Its staff harmonized and purified information among the systems to ensure proper model behavior. To make the predictive analytics models at MedCare clinically relevant, predictive analytics specialists design and validate the models and retrain them continuously. The organization minimizes the financial implementation cost as it provides scalable and cost effective solutions. Above all, predictive insights are ingrained in the system of the revenue cycle and clinical workflow, giving MedCare the ability to deliver actionable intelligence to appropriate teams at the appropriate time, enhancing the performance of the organization, financial results, and the overall functioning of the entity.

